
Multiple Sclerosis During the Covid-19 Pandemic

It’s undeniable that the Covid-19 pandemic has had a significant impact on the treatment of a lot of, if not all long-term and chronic conditions.
Here, we explore the impact that Covid-19 has had on Multiple Sclerosis (MS) activity in the inpatient setting, using Hospital Episode Statistics (HES) data collated in Meditrends, our online real-world data business intelligence platform.
Meditrends provides detailed analysis and interpretation of aggregated and anonymised HES data, helping HCPs and pharmaceutical professionals define, refine and inform healthcare decisions and improve health outcomes.
Hospital Episode Statistics (HES) data
Hospital Episode Statistics (HES) is a database containing details of all admissions, A&E attendances and outpatient appointments at NHS hospitals in England. It allows hospitals to be paid for the care they deliver (Payment by Results).
Each HES record contains a wide range of information about an individual patient admitted to an NHS hospital. For example:
- clinical information about diagnoses and operations
- information about the patient, such as age group, gender and ethnic category
- administrative information, such as date of admission, treatment speciality
- geographical information on where the patient was treated and the area in which they lived.
Primary inpatient admissions – patients with a primary diagnosis of MS
A primary admission indicates the reason for the admission – the primary diagnosis.
Unfortunately, HES data coding does not allow us to distinguish between the different types of MS – clinically isolated syndrome (CIS), relapsing-remitting MS (RRMS), secondary progressive MS (SPMS) and primary progressive MS (PPMS). However, it does still offer some valuable insights.
As can be seen on the graph below (taken from Meditrends), in January 2020 there were 5,510 primary admissions for MS, which reduced to just 3,200 at the height of the pandemic and first lockdown in April 2020. There was a slight increase in the number of primary admissions as restrictions following the first lockdown were relaxed; July saw 5,045 primary admissions, but since then the number of patients being admitted with a primary diagnosis for MS reduced again to 4,285 in August and 4,670 in October 2020.
It is worth noting that October’s data will include incomplete admissions – where a patient was still in hospital at the end of October when the data was submitted.
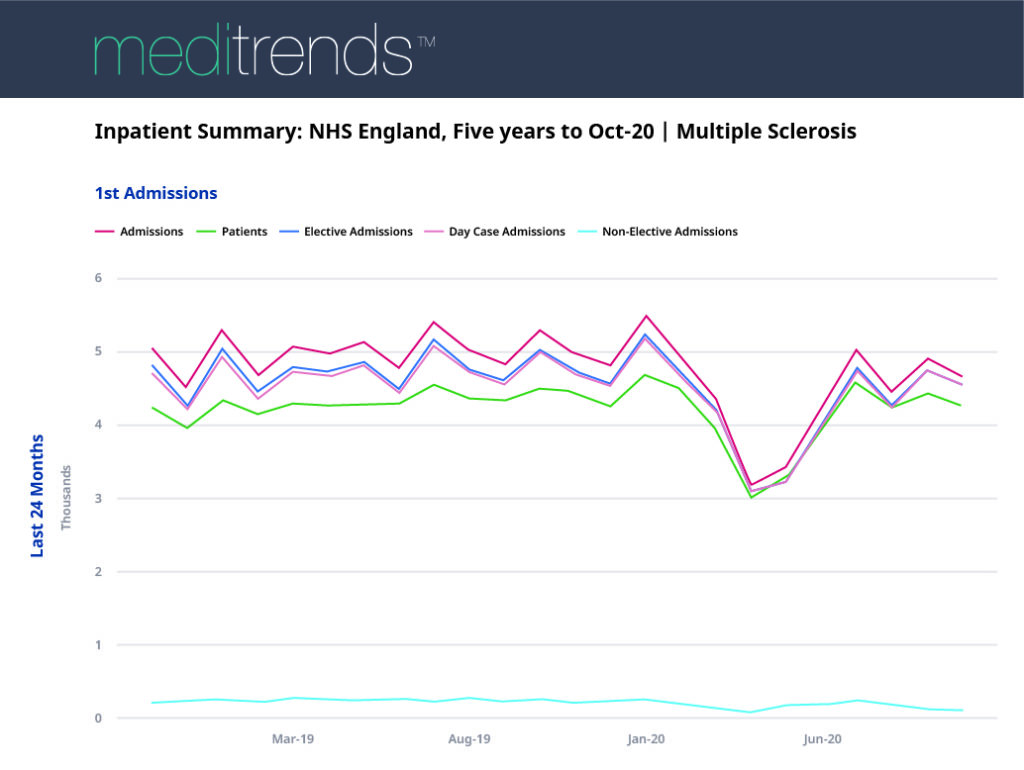
As shown on the graph above and the two graphs below, the number of non-elective admissions for MS is consistently low, pre-pandemic and during the pandemic, so it is mainly day case and elective admissions that have been impacted.
Elective admissions
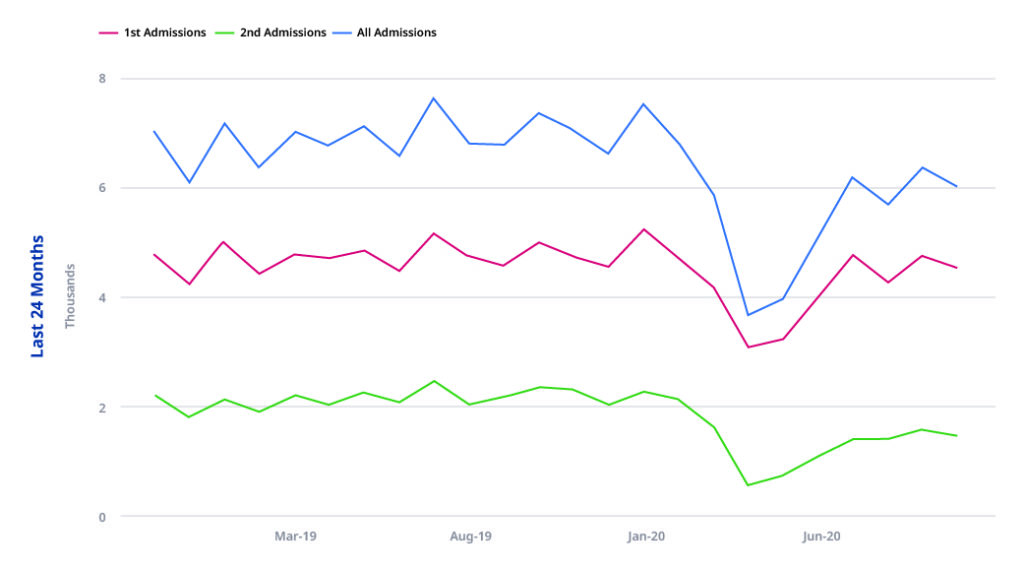
Day case admissions
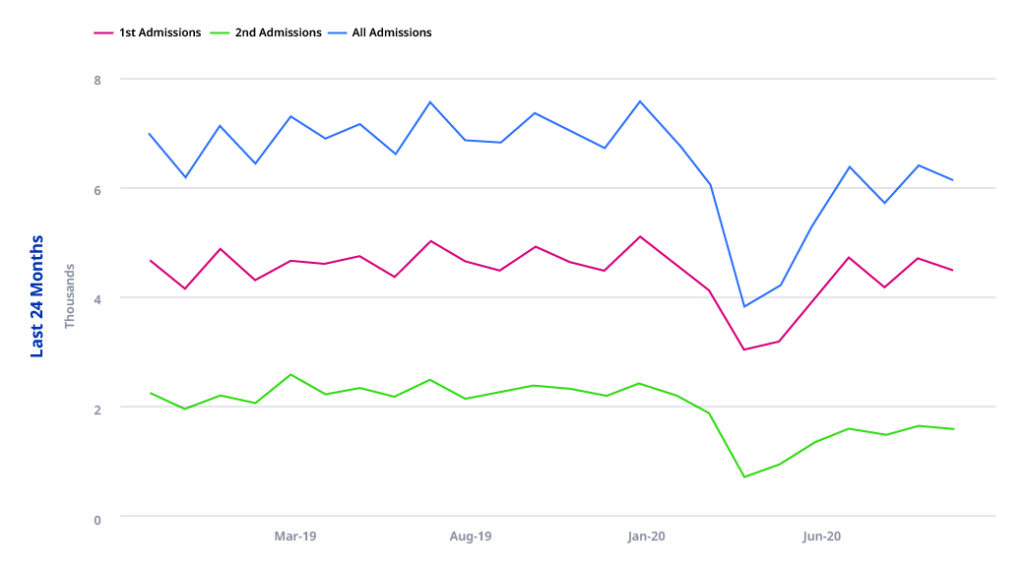
Inpatient admissions for patients with MS in any diagnosis position
‘Any diagnosis position’ means that MS was captured as either the primary diagnosis or as one of 20 ‘other’ diagnoses that are recorded for each patient admitted to hospital.
Inpatient admissions for patients with MS in any diagnosis position have been similarly impacted by the COVID 19 pandemic.
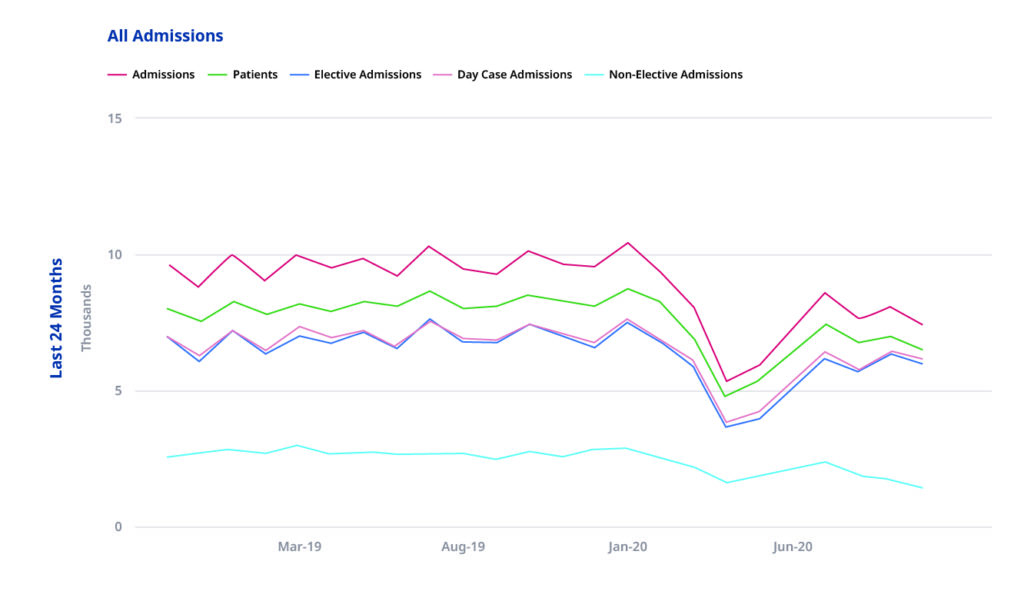
We can see from the graph above that in January 2020, pre-pandemic, there were 10,435 admissions for patients with MS in any diagnosis position, which reduced dramatically to just 5,390 in April 2020. July saw numbers increase to 8,630 admissions, but in October this had reduced to 7,470 admissions.
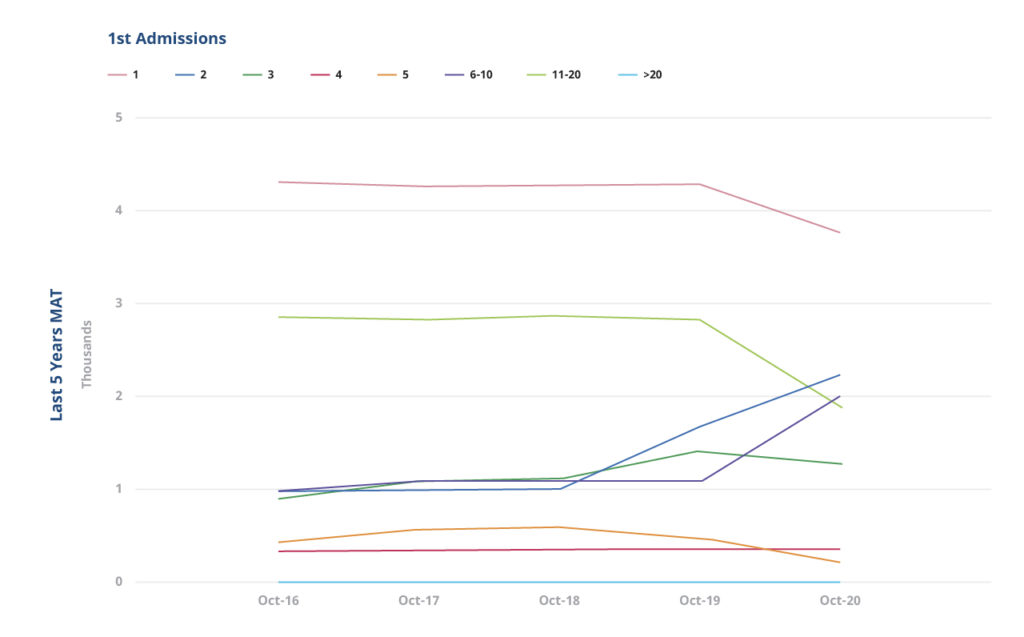
Admission Frequency
Admission frequency looks at the number of admissions per patient. Whilst we can see from the graph below that single admissions are most common, there are a large number of patients being admitted more than once. This is most certainly due to multiple day-case admissions for treatments such as infusions.
Prevalence
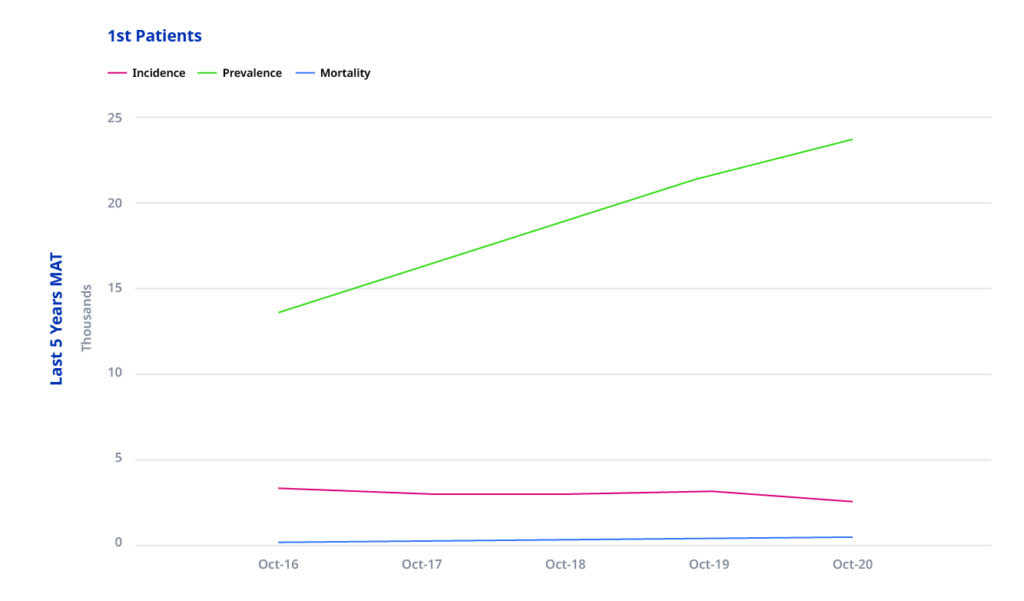
Prevalence relates to the number of patients (who are still alive) who have had a primary diagnosis of MS in the past five years. To calculate prevalence we use the last five years of data, and prevalence figures stated are cumulative. Note that prevalence is calculated based on inpatient admissions, so if an MS patient has not been admitted, they will not be included in this count.
We can see from the HES data in the below graph that prevalence of patients with a primary diagnosis of MS has increased from 13,705 patients in October 2016 to 23,775 patients (cumulative) in October 2020.
Mortality
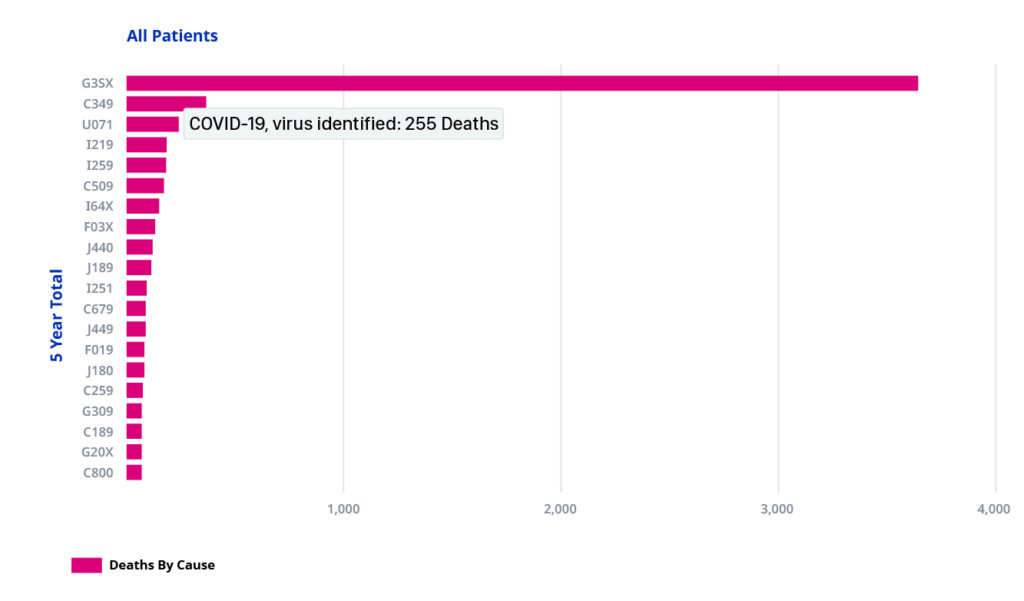
Meditrends also shows us that the leading cause of death in admitted patients with a diagnosis of MS in any diagnosis position is ICD10 code G35X, which is the code for MS.
ICD10 code U071, which is the emergency code used for Covid-19, is listed as the third highest cause of deaths in the last five years, with 255 deaths attributed to this code.
In Summary
The ability to see inpatient hospital activity across all diagnoses and procedure codes shows particular therapy areas clearly in the context of the whole NHS – whilst reporting on secondary and primary diagnoses, as well as elective vs planned admissions, gives a true picture of the burden of disease.
Meditrends provides an invaluable resource for any NHS or pharmaceutical professional wishing to understand more about the demographics of their disease area – giving users unparalleled access to anonymised and aggregated HES data.
Without knowing when and how patients present at hospital with a particular condition, efforts at planning for all aspects of your strategic and operational process, for example, often involve guesswork. However, Meditrends can give you invaluable insights that you know are based on reality.
To find out more about the impact Covid-19 has had on patients with a diagnosis of multiple sclerosis – or to obtain similar insights relating to your disease or therapy area – please contact Sarah Brooks (Sarah.brooks@dice-comms.co.uk).






